 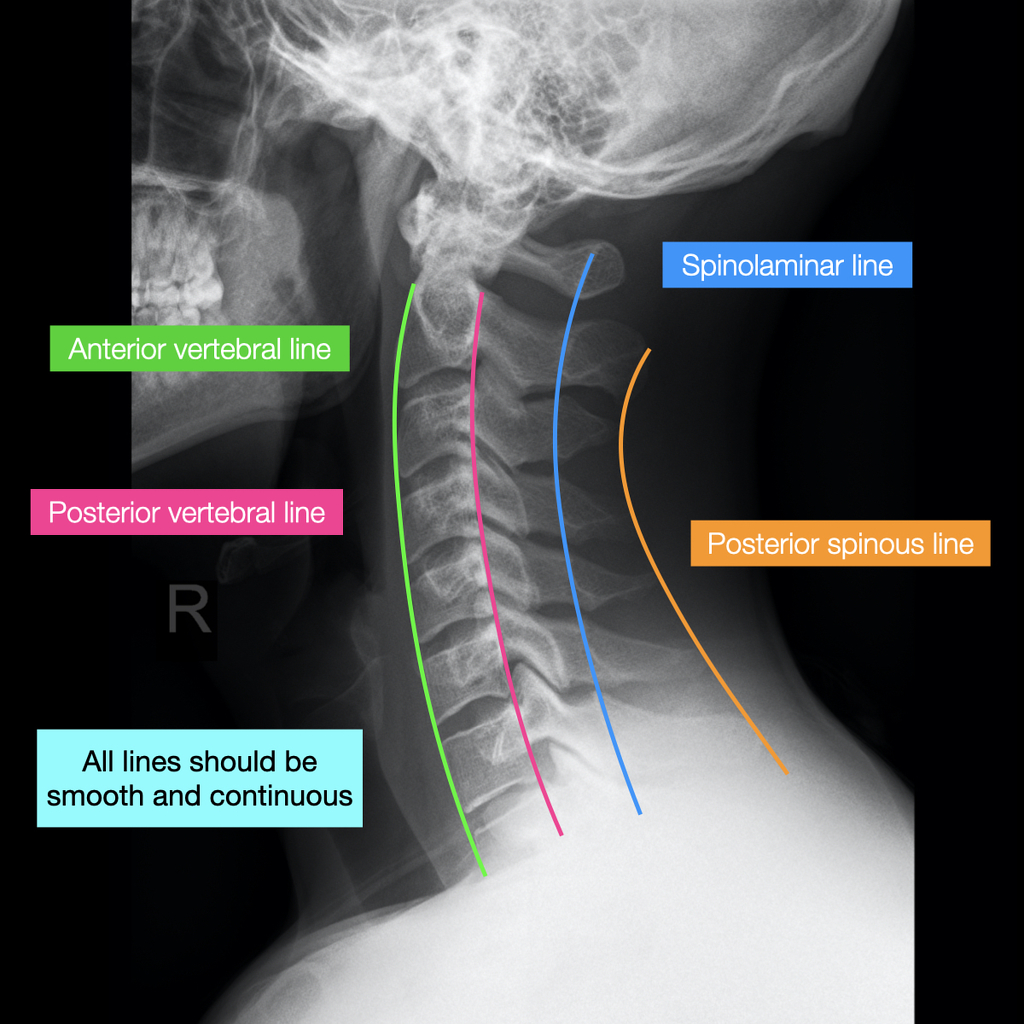
Using a 45° radiolucent sponge in the supine position will assist the patient in maintaining the correct position, whilst flexing the knees will also provide stability.Įxpiration (to minimize superimposition of the diaphragm over the upper lumbar spine)Ģ.5 cm above the iliac crests and 3 cm lateral from the spinous processes towards the upside. RAO and LAO will demonstrate the facet joints on the upside, for example, the LAO position will show the right facet jointsĢ.5 cm above the iliac crests and 5 cm medial from the ASIS on the upside. Two radiographs performed with patient at RPO 35-45° and LPO 35-45°Įnsure arms are removed from the region of interest Two radiographs performed with patient at RAO 35-45° and LAO 35-45° The radiographs can be performed with the patient in the posteroanterior (PA) erect or supine position This retrospective study involved cervical spinal MRIs of 96 patients aged over 60 years. Smooth and continuous and that C2 does not appear "fat" (i.e.This view is used most commonly to assess for a pars interarticularis defect, although this has largely been superseded by CT and MRI. Additionally, it is a frequently used view for needle placement in fluoroscopic guided procedures 2, such as transforaminal epidural steroid injections. Cervical NFS is known to be common in older age groups because degenerative changes in the cervical spine are the most common cause of cervical NFS and degenerative changes increase with increasing age (14, 15, 16). CERVICAL SPINE Body Part Grid mAs CM kVp AP/Oblq Cervical/ Y 3.5 4-5 72 7 10-11 76 14 16-17 82 44' 5.25 6-7 72 10.5 12-13 76 21 18-19 82 7 8-9 72 14 14-15 76 28 20-21 82 Grid mAs CMkVp mAs kVp mAs CM kVp LATERAL Cervical Y Same Increase 4 44' Grid mAs CM kVp mAs CM kVp mAs CM kVp LATERAL Cervical Y 16 4-5 72 32 10-11 76 64 16-17 82 at 72. Make sure the basion-dens space is Make sure the atlantodens interval (ADI or pre-dental space) is Check that the intervertebral spaces are uniform at each level.Surface of the occipital and sphenoid bones) detail, against a uniform background) the ideal x-ray spectrum is Monochromatic. Clivus should be pointing toward the odontoid (the clivus lies at the base of the skull is made from the.Inspect each vertebral body, pedicle, lamina and spinous process from C1 - C7 Check the posterior vertebral line (posterior longitudinal ligament line).Check the anterior vertebral line (anterior longitudinal ligament line).Lordosis means there is a distinct curve in the neck when. Evaluate the orientation of the epiglottis, hyoid bone, tracheal shadow and check for any foreign bodies When viewed from the side, a typical cervical x-ray (neck x-ray) has a curvature called lordosis.Vertebral body) and < 22 mm in front of C6 (or no more than width of C6 Tissue is < 7 mm in thickness in front of C2 (or < 50% of the width of C2 Make sure you can see all 7 cervical spinous process.The clinician should establish a process or order they follow each time. To the tip of the dens (or odontoid process). superiorly to include the C7/T1 junction inferiorly to include the T12/L1 junction lateral to include the costotransverse joints and left and right paraspinal lines orientation portrait detector size. The dorsal surface of the clivus and is used to measure the distance of space the central ray is perpendicular to the image receptor collimation. This is a line drawn from the caudal extension of The tip of the dens should lie less than 4.5 cm above this line. Draw a line from the posterior edge of the hard palate to the caudal end of the occipital curve. Opisthion (posterior aspect of the foramen magnum) cannot be identified on a To recognize the presence of basilar invagination (a craniocervical junctionĪbnormality where the tip of the dens project up into the foramen magnum). If the tip of the dens extends > 3 mm above this line then it helps.The odontoid tip extends above this line. Posterior surface of the hard palate to the tip of the opisthion (posteriorĪspect of the foramen magnum) and is used to measure the distance of how much (normal CT values for men is > 23.7 mm and for women is > 24.2 mm) can be used instead. Tip of the dens is eroded then the Redlund-Johnell and modified Ranawat methods The dens (or odontoid process) should be ~5 mm below this line. Lateral radiograph of the skull or on a sagittal cut from a CT or MRI scan thatĬonnects the posterior and anterior aspects of the foramen magnum. Note: Scroll over or tap on the image to see labels & lines 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
